What are Moving and Handling Policies in Health and Social Care: Guidance on Equipment
Moving and handling is a key part of the working day for most employees in health and social care; from moving equipment, laundry, catering, waste or supplies, to assisting service users in moving. To ensure moving and handling is done correctly and safely, there are various policies and pieces of legislation you must follow.
This article includes information on what moving and handling is and the types of equipment that are often used. It also covers the policies that are in place and the legislation involved, as well as the importance of risk assessments.
What is Moving and Handling?
Moving and handling refers to the manual handling of people. In the past, it was often referred to as just manual handling, however it is now known as moving and handling to differentiate between the movement of objects and people.
Before being able to move people in a care setting, you must be fully trained. This often involves learning and practical training before an assessment of competency is completed.
Want to know more?
If you work in health and social care, why not check out our Moving and Handling People in Health and Social Care course? This course covers the information and guidance needed to move and position service users safely and the importance of risk assessments, as well as the potential hazards and injuries involved.
If you work in health and social care, you will probably be involved in moving and handling people. This encompasses any time you support someone to move and will often involve the use of specialist equipment.
Some examples of activities that you may not think involve moving and handling, but actually do, include:
- Helping a person in and out of bed, to turn over or to sit up.
- Helping a person go to the toilet.
- Helping a person to wash or bathe.
- Helping a person to stand, walk or sit down.
- Helping a person get in or out of a car.
- Lifting and carrying loads of laundry.
- Pushing, pulling or carrying cleaning supplies.
- Moving furniture or other objects.
- Bringing objects to a person’s chair or bedside.
- Carrying food trays or pushing a food trolley.

If not carried out correctly, moving and handling activities can cause serious physical injury to you and others. Therefore, it is important you follow your training and an ergonomic approach.
As well as ensuring you move and handle individuals safely, you also need to use and maintain equipment correctly. Many types of equipment are vital for certain moving and handling tasks in order to prevent injuries whilst promoting independence, dignity and quality of life.
Types of Moving and Handling Equipment in Care
Staying safe during moving and handling activities is paramount, therefore there are many considerations when dealing with different types of equipment. In the past, health and social care workers used techniques that required the care worker to support most of the service user’s weight, which led to many injuries.
Moving and handling techniques now involve the use of specialist equipment to reduce the physical impact on those involved and the likelihood of injuries.
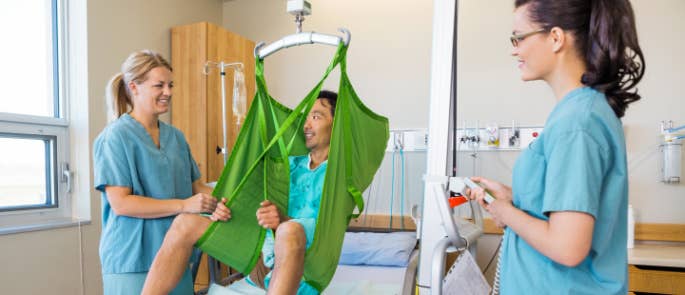
Before you use moving and handling equipment, there are certain checks you must carry out to ensure the safety of those involved. You should ask yourself:
- Are there any signs of damage such as cracks, frays or exposed wires?
- Is the equipment clean?
- Has electrical equipment been serviced and had an up-to-date portable appliance test (PAT)?
- Is there enough charge in the equipment to carry out the task?
- Are there any trailing wires?
- Is there enough room to complete the task?
- Have the members of staff been trained and deemed competent to use the equipment?
- Is the equipment appropriate for the individual, such as the correct size?
Necessary equipment may include:
Hoists – there are several variations and types of hoists available, they are generally used for those who are non-weight bearing and include mobile hoists (these are brought to the service user and used to transfer them), ceiling or tracking hoists (these have a motor that moves along a track on the ceiling from which a cradle can be lowered or raised on a lifting tape), standing hoists, bath hoists or bath lifts.
Slings – there are many variations of slings including bath slings, toilet slings, in-situ slings (these are used when removing the sling is difficult due to fragile skin) and transfer slings.
Slide sheets – these are sometimes referred to as glide sheets and are made of a low-friction material. They are used to help move an individual with less physical effort and without dragging. Some are permanently underneath the service user, others are only placed underneath them during manoeuvres, some are disposable and others are reusable.
Transfer boards – these are used to assist in moving a service user to and from different furniture, for example from a seat to a wheelchair. They are often used in conjunction with slide sheets or handling belts.
Turning aids – these are used to assist in turning people around and are also known as rota stands, turntables or patient turners.

Electric profiling beds – these are mostly for dependent or immobile residents and provide adjustable height and tailored positioning of the individual while in bed. They are used to adjust the bed for eating, breathing issues or to move the individual from a seating to standing position.
Wheelchairs – wheelchairs are very common in health and social care and come in a variety of types. They may be electric, manual, able to recline and or very basic.
Handling belts – these are used for assisting residents who can support their own weight to help them stand up. They should not be used for lifting.
Bed levers – sometimes referred to as support rails or poles, these do not strictly class as moving and handling equipment however they are worth mentioning. They are used to reduce the risk of falls and aid the service user when repositioning in their bed.
Moving and Handling Legislation
There are various pieces of legislation that outline the requirements for moving and handling. Following legislation and guidelines is essential to ensure employees and service users are safe.
Legislation focuses upon reducing risk through the use of risk assessments. This is especially important in moving and handling as there is a high risk of injury to both staff and service users if an activity is carried out incorrectly.
There are a few different pieces of legislation that are involved, including:
- The Health and Safety at Work etc. Act 1974.
- The Manual Handling Operations Regulations 1992.
- The Management of Health and Safety at Work Regulations 1999.
- Provision and Use of Work Equipment Regulations 1998 (PUWER).
- Lifting Operations and Lifting Equipment Regulations 1998 (LOLER).

If moving and handling activities are carried out without following the legislation and guidance given, those involved are at a high risk of injuring themselves or others. Consequently, employers should put in place their own policies surrounding moving and handling to ensure legislation is being followed.
What is the Moving and Handling Policy in Health and Social Care?
As mentioned, there are policies in place within health and social care settings which can help carers to safely move and handle their service users.
Some key elements of a moving and handling policy include:
- A statement of the organisation’s commitment to managing the risks associated with moving and handling people and loads.
- Details of who is responsible for doing what.
- Details of your risk assessment and action planning processes.
- A commitment to introduce measures to reduce the risk.
- Arrangements for training.
- Arrangements for providing and maintaining handling equipment.
- Details of your systems for monitoring compliance with the policy and for regular review.
- Information for staff on reporting pain and injuries.
Moving and Handling Risk Assessment for Carers
Even with policies and procedures in place, a risk assessment is still needed. Risk assessments are a legal requirement and evaluate the risks involved in moving and handling activities, then put in place ways to reduce them in order to prevent harm to service users or staff.

The main steps involved in a risk assessment are:
Identifying the hazards – this means identifying the possible risks to health during moving and handling activities, such as excessive strain or awkward positioning. The risk assessment should also identify the type and frequency of moving and handling activities, the equipment used, the staff involved and the environment, including moving and handling in the event of emergencies such as fire evacuations.
Identifying who may be harmed and how – this means identifying the people at risk of harm from the hazards involved in moving and handling. This will include the staff, service users and any visiting family and friends.
Evaluating the risks – risk assessments must be tailored to the individual’s specific needs and should consider their abilities, the equipment to be used, the number of staff needed and moving and handling in case of emergencies, such as a fall. It should be taken into consideration that the individual’s needs and abilities can change over time and even during the course of a day, for example if they take a medication that affects their muscle strength.
Controlling the risks – this step involves deciding on the precautions that will be taken to reduce the likelihood of harm. One of the first considerations should be whether the moving and handling activity is absolutely necessary. If it is not possible to remove the need for moving and handling, appropriate control measures should be put in place.
Recording and reviewing the assessment – if there are five or more members of staff within a care provider, it is a legal requirement to record the findings of risk assessments. However, regardless of size it is good practice to keep a record of risk assessments. They should be reviewed regularly, especially in the event of new equipment, a new service user, procedural changes, if an accident occurs, or if the health of the service user changes significantly enough to impact on the risk assessment.
You should familiarise yourself with the risk assessments, policies and procedures within your care setting to ensure you are working in the safest way. As well as following risk assessments and legislation, you should read through individual care plans before performing any moving and handling activity to guarantee the action you are about to perform is appropriate and necessary.
There are a multitude of different moving and handling techniques that often involve the use of specialist equipment. Moving and handling equipment varies and you should ensure it is safe and you know how to use it to prevent injury to anyone involved in the activity. Risk assessments and legislation are in place to keep everyone safe and should be followed so you can provide high-quality care.
Further Resources:
- Moving and Handling People in Health and Social Care Training Course
- Ergonomic Approach to Manual Handling in Care Homes
- Manual Handling in Care Homes
- Health and Safety in Care Homes: Free Audit Template
- Basic Life Support Training








