What Methods Can Be Used for the Disposal of Infectious Waste?
Cleaning and disposing of infectious waste isn’t a role for the squeamish. You work in close proximity of blood and other bodily fluids – as well as waste materials – which may carry common infections (like HIV, hepatitis, and meningitis to name a few).
But your job is a vital one. Improper disposal poses a high risk of you or others being exposed. Contracting a disease starts the chain of infection all over again, and allows the disease to keep on spreading.
If you clean for an organisation that works with people or animals (and their bodily fluids), you’ll need more than a mop and bucket on hand.
Proper disposal methods and hygiene are of paramount importance.
What is Infectious Waste?
Infectious waste includes any fluids, solids, or materials that have the potential to carry infectious microorganisms and transfer diseases.
The World Health Organisation’s (WHO) definition of infectious waste is:
“Waste contaminated with blood and its by-products, cultures and stocks of infectious agents, waste from patients in isolation wards, discarded diagnostic samples containing blood and body fluids, and contaminated materials (swabs and bandages) and equipment (such as disposable medical devices).”
Infectious waste is anything contaminated with human and/or animal:
- Blood.
- Bodily fluids, e.g. saliva, mucous, or pus.
- Waste products (faeces, urine, and vomit).
- Skin or tissue.
These can contaminate all sorts of surfaces and materials.
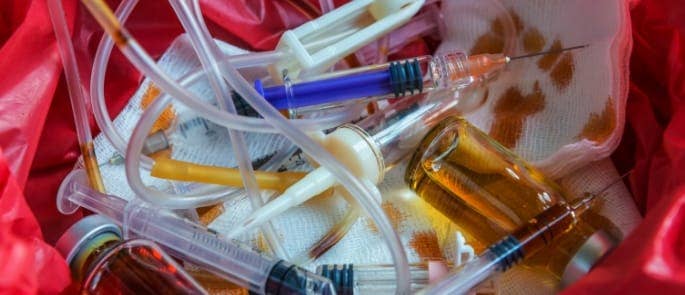
Items that pose a risk to cleaners and people in charge of waste disposal include syringes and needles, scalpel blades, plasters, bandages, soiled clothing, bedding (human and animal), toilets, materials used to clean wounds, and sanitary waste (e.g. feminine hygiene products or incontinence pads).

Spillages of infectious waste pose an immediate and direct risk; it’s essential that you clean it up and sanitise the area thoroughly. And remember: anything can become contaminated. A mug, a blanket – any basic object.
You cannot clean a contaminated item as you normally would. Remove it safely from the premises, i.e. without posing a risk to yourself and others in the process, and dispose of it appropriately (no dumping it in the nearest bin).
This isn’t just a case of best practice; it’s a necessity. It’s the law.
Need a Course?
Our Infection Prevention & Control (IPC) Training covers the sources of microorganisms and how infectious bacteria transfer between hosts. Learners will understand the process of preventing infections from spreading.
Highly Infectious Waste
When you work in a risky environment like a healthcare setting or work with animals, you must act as if everything you handle and clean is infectious. Because at a first glance, it’s impossible to tell the difference between what’s gross (but harmless) and what’s carrying a disease.
However, in some settings you’ll be told which waste materials are categorically carrying infection – and in a dangerous amount.
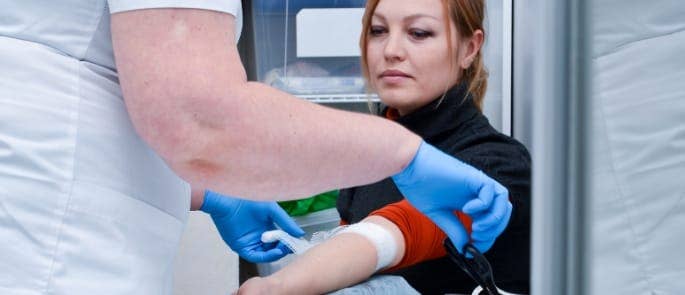
This is referred to as highly infectious waste.
Highly infectious waste is usually only present in controlled environments: where microbial organisms are deliberately allowed to multiply (for example in laboratories). But it also refers to the body fluids of people known to be carrying highly infectious diseases, which may be present in a medical setting.
It’s unlikely you’ll need to work around highly infectious waste, but if you do you’ll be given explicit instructions specific to your premises for handling and disposing of it.
Improper Disposal of Medical Waste
You can guess what happens when you don’t dispose of infectious waste properly: people are at greater risk of harm.
According to the WHO, 85% of waste generated by healthcare settings is general, non-hazardous waste. But 15% is potentially infectious.
This waste could contain harmful organisms that, if given opportunity, may infect other patients, staff, and the general public – and spread beyond your premises. It is a huge risk to vulnerable people in a medical setting, i.e. those already ill, new-borns, and the elderly: infections hit them with even greater force.
Improper disposal could even result in the release of a drug-resistant disease into the environment, which can spread to people unaware of effective infection control and become difficult to contain.
Needles and syringes not disposed of properly can cause a sharps-inflicted injury and transfer an infection. The WHO states that someone who experiences one needle stick injury from a needle used on an infected patient has a 30%, 1.8%, and 0.3% risk of contracting HBV, HCB, and HIV respectively.
The environment could also suffer due to improper disposal – it could cause poisoning and pollution through waste water or toxic elements or compounds released during incineration of infectious waste.
Safe Disposal of Medical Waste
First and foremost: follow any training provided on how to safely dispose of materials in your premises. Your setting may have specific procedures in place with which you should be familiar, and may provide you with specific equipment and substances for sanitisation and disposal.
General steps for safe disposal:
- Wearing protective equipment.
- Proper cleaning procedures for contaminated surfaces.
- Proper sanitisation or disposal.
Wearing protective equipment
Infections spread easily through physical contact; hands are one of the most common vehicles of infectious bacteria.
You must wear protective gloves when handling waste. Do not touch anything other than the infectious waste once you have put them on, and make sure you remove and dispose of them hygienically once you’re done. Dispose of them like you would any other infectious waste unless told otherwise.

Also, cover your body as much as possible. This is especially important if you have any open wounds (even a tiny cut on your hand could be enough for entry). Properly dress wounds with sterile plasters or bandages.
Cleaning contaminated surfaces
A quick wipe down of a surface may look like it’s removed all infectious substances, but microorganisms are guaranteed to linger if it hasn’t been sterilised.
Be sure to isolate the area, use suitable cleaning substances such as a chlorine releasing agent, bleach, hot water, and detergent, and dispose of all materials used to remove the substance (including gloves) hygienically and safely.
Be sure to sanitise your hands afterwards (yes; even if you were wearing gloves.)
Proper sanitation or disposal
Your setting will have certain procedures for moving, removing, or destroying infectious materials. Consider all stages: from storage, through handling and bagging, to transportation and laundering.

- Minimise contact, i.e. handle materials as little as possible and transfer them via routes that minimise exposure to others.
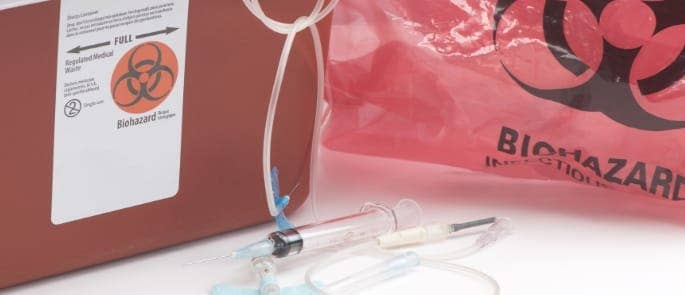
- Discard materials into a suitable container or bag. It must conform to the required standards (e.g. UN approved).
- Use bags that are marked or coloured for infectious waste. This includes orange or yellow bags (or signs), and text or symbols indicating the bag contains hazardous waste for treatment or incineration.
- Transfer non-disposable infectious materials safely to the sterilisation department for decontamination. You must adhere to the local policy for cleaning the equipment.
- Always use puncture-resistant containers sharps, as they will not leak.
- Use pierce-proof waste containers and close them in between use for safety.
- Never fill a bag or container more than ¾ full.
- Never over fill waste receptacles.
- Remove waste in accordance with local clinical waste disposal policy; it may be collected by the relevant authorities, removed by an infection control team, or incinerated.
Whatever waste you are handling, it’s imperative that you follow the procedures instructed of you and minimise direct contact. This ensures you break a link in the chain of infection and stop the spread of infectious diseases.
Further Resources
- Infection Prevention & Control (IPC) Training
- Ten Tips for Infection Prevention and Control
- Sharps & Needlestick Risk Assessment Template
- What Are the Different Types of Healthcare Waste and Why Are They Important?
- Hand Hygiene and Infection Control Quiz







