Child Protection Body Map
There are many different ways in which a child can be abused. One of the main four types of abuse that a child can face is physical abuse. Physical abuse is any kind of intentional abuse that causes physical harm to a child. The signs of physical abuse are not always as obvious as you may think as bruises can be explained away by clumsiness typical of young children or carefully hidden by clothing.
Anyone who has a responsibility for safeguarding children must be able to recognise the signs of abuse and know what to do once those signs have been identified. A child protection body map can help to record a child’s injuries and can play a vital role in building a picture that may indicate abuse and lead to the necessary action being taken to protect a child. In this article we will outline what a child protection body map is and how you should use one. We will also provide you with a free downloadable child protection body map template that you can use in your setting.
What is a Child Protection Body Map?
A child protection body map is a visual record of physical abuse. Body maps are used to document physical injuries that a child may have, especially if it is felt that the injury is non-accidental or part of a larger pattern. As well as documenting the frequency and location of an injury, child protection body maps help professionals to work together when deciding whether there is a safeguarding issue.
Body maps are a record of what can be seen and/or what has been said about an injury. It’s important to note that the use of a body map does not replace medical advice and a proper diagnosis of the injury and correct treatment should be sought by a medical professional where necessary.
When recording a child’s physical injuries you must never photograph the child.
Body Map for Safeguarding
Physical abuse is abuse that causes physical harm to a child. It is intentional abuse that seeks to cause pain and harm and may involve hitting, shaking, throwing, poisoning, burning, drowning, suffocating or otherwise causing physical harm to a child. Children are prone to accidents and not every injury is indicative of a child being physically abused. This means that physical injuries can often be dismissed as a ‘one-off’ or a series of accidents that do not need to be taken any further. It is therefore vital that all signs of abuse are documented, irrespective of how seemingly small they are, as it may point to a larger issue that needs addressing.
Child protection body maps are invaluable tools for documenting physical abuse as well as when attempting to assess whether physical abuse is occurring. They provide an insight into what a child may be experiencing by highlighting potential patterns or unconvincing justifications for injury. As such, it’s vital that body maps are as informative as possible and include details pertaining to:
- Who noticed the injury and their relation to the child
- When the injury was noticed
- Details of the injury – this should include where it is on the child, what it looks like, the colour, shape, size and condition of the injury
- Whether the injury is getting better or deteriorating
- Whether the child is in distress or indifferent about the injury
- Any explanation given for the injury from the child and/or parent or carer
- How the child is feeling and what their behaviour is like

It’s advisable to include both a drawing and a written description of the injury when completing a child protection body map.
As mentioned, children are prone to injury and a solitary incident of injury does not indicate physical abuse. However, accidental injuries often occur in different places than intentional injuries. For example, a child having a scraped knee could easily be explained by them falling while playing with friends. Comparatively, lash marks across the back of the thighs are far less likely to be an accident.
The NSPCC notes the following as patterns and locations of bruising that may indicate physical abuse is taking place:
- Bruising on soft parts of the body such as the abdomen, back and buttocks.
- Bruising on the head, ear and neck.
- Bruising as a result of self defence on the forearm, upper arm, back of the leg, hands or feet.
- Clusters of bruises commonly found on the upper arm, outside of the thigh, or on the body.
- Bruises which have petechiae (dots of blood under the skin) around them.
- Bruises that carry the imprint of the implement used or a hand.
- Severe bruising to the scalp, with swelling around the eyes and no skull fracture may indicate a child has been ‘scalped’ i.e. had their hair pulled violently.
Other common sites for non-accidental injury include:
- Cheeks
- Mouth
- Shoulders
- Chest
- Genitals
All types of injury should be drawn onto a child protection body map, even those that appear to be accidental or a natural part of a child’s development. What may seem insignificant or accidental now, may become important in the future and provide clear evidence of abuse.
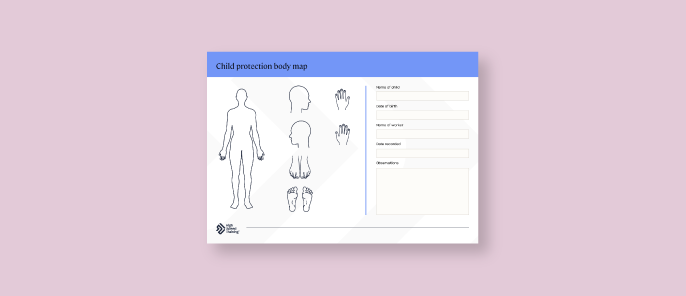
Child Protection Body Map Template
Documenting signs of child abuse can be difficult. It can be hard to know what to include and personal feelings rooted in wanting to protect a child can make objectivity hard. A child protection body map supports those with safeguarding responsibilities to record accurate and objective concerns.
Below you will find a child protection body map template that you can use in your establishment. The body map should be used to record and describe injuries. Remember, you must not photograph a child’s injury. Instead, you should use the outline provided to draw the injury as best you can. You can also use the observations section to add any additional descriptions, the behaviour of the child and the explanation they may have given for the injury.
When completing a body map it’s important to consider the following:
- A child that is being physically abused may ‘fawn’ as a defense mechanism, not recognising that they have the right to consent. Ask the child for their consent to record what has happened to them. You should also seek out consent from a parent or guardian. If this is not suitable given the situation, discuss the circumstances with the designated safeguarding lead (DSL) who can offer further guidance.
- Ensure that another adult is present during the reporting. A good system is to have one adult make notes whilst the other asks questions. This ensures that focus can be directed towards the child, rather than being split between listening and documenting all important information.
- Make sure any descriptions are as detailed as possible and where possible include information on the colour, size and dimensions of the injury. You should also make note of any foreign bodies present in the injury such as gravel or lint as this can help to clarify whether the injury was accidental or caused by something else.
- Use the child’s own words where possible and ensure that your own observations are objective.
- If a child discloses an injury that is covered by clothing, do not ask them to remove the clothing to show you. Explain that you do not need to see it to believe them or make a note of the injury and ask them to describe the injury as best they can.
- Only document what you can see or what you have been told, don’t try to infer meaning from it. It’s also important to not ask leading questions such as ‘did someone at home hurt you and cause that bruise on your arm?’ Instead keep it simple and ask ‘what happened to your arm?’ Children who are being physically abused are often very hesitant to discuss it and there are a myriad of reasons why they may not disclose that they are being abused. Comparatively, a child that has injured themselves accidentally is unlikely to shy away from discussing how it happened.
What to do After Filling in a Body Map
After completing a child protection body map a decision must be made on whether there is an immediate risk to the child and whether they need to be taken for treatment for their injury. If you suspect that a child is in immediate danger, you must call the police on 999 straight away. If you conclude that a child should be taken for treatment for their injury, discuss this with your DSL and follow your establishment’s relevant policy.
You should report any concerns you may have about a child’s safety, regardless of how small it may appear. Upon completing a body map you may worry that you have overreacted or that the given explanation is, upon consideration, reasonable. Nevertheless, you should report any concerns that you have as this can highlight a pattern of abuse that may otherwise go unnoticed. You can also seek advice from others if you are unsure. This could be from colleagues who may have similar concerns or from professionals such as the NSPCC. The NSPCC has a wide range of information and advice for anyone worried about a child’s safety and contacting them can provide an invaluable professional perspective that will guide your next steps. The NSPCC is available 24/7 and can be contacted by calling 0808 800 5000.
If it’s appropriate to do so, and you do not suspect that they have caused the injury, you should also share your observations with the child’s parents or carer so that they understand what decisions have been made and why. It’s also important that you maintain open communication and an ongoing relationship with the child. Children who are being subjected to abuse often isolate themselves and this can make it easier for the abuse to continue as they have no one to turn to for help. Moreover, if you noticed the injury rather than them disclosing it, they may be fearful of the ramifications and withdraw even more. Maintaining an ongoing relationship with them reassures them that you have a vested interest in their safety and that you are an adult that they can trust.

Abuse of any kind can have incredibly harmful, life long consequences for a child. Whilst abuse can be hard to spot, physical abuse has one of the more obvious visual markers and so it’s vital that these markers are not ignored or dismissed. A child protection body map is a useful means to objectively document a child’s injury and assess any safeguarding concerns that must be addressed.
Further Resources:
- Signs of Abuse in Children
- Understanding Why Children May Stay Quiet About Abuse
- Safeguarding Courses











